
A Guide To Repairing Family Relationships
Discover expert tips for repairing family relationships and fostering healthy connections with The Recovery Team.
If you or a loved one are struggling with addiction, you may be concerned about the financial burden of getting the help you need. Understanding what types of addiction treatment are covered by insurance and what your insurance policy includes is an important first step toward getting the support you need.
In this article, we will explore the different types of insurance coverage available for addiction treatment and provide information on how you can use your insurance benefits to pay for treatment at our facility. Our goal is to help you make an informed decision about addiction treatment and alleviate any financial concerns you may have.
At The Recovery Team, we strongly believe that everyone should have access to substance abuse treatment without barriers. We understand that quality care is not only essential but also liberating. We strive to provide effective and affordable services to our clients while ensuring that insurance coverage is available to those who need it.
If you or a loved one is in need of help, our confidential counselors are available to answer your questions, provide details about our services, and assist with verifying insurance benefits. Contact us today to take the first step toward recovery.
The coverage for addiction treatment programs through insurance can vary significantly based on different factors such as the employer, specific insurance plan, and the type of rehabilitation program required. Despite the differences, it’s important to understand that substance abuse is classified as a federally recognized medical condition, and hence, most insurance plans are required to cover addiction treatment programs.
However, the extent and nature of the coverage can differ significantly based on the type of plan, and the level of coverage offered by an employer. Therefore, it is critical to carefully review the details of an insurance plan, its coverage for addiction treatment, and any potential costs associated with the treatment before making a decision.
If you are unsure whether your private insurance covers addiction treatment, we encourage you to reach out to The Recovery Team today. Our admissions staff is available to assist you in understanding the specifics of your insurance plan’s coverage and our rehab center’s payment options. In most cases, health care insurance covers a significant portion, if not all, of the costs associated with addiction and mental illness treatment.
We can provide you with the necessary information to make an informed decision about seeking treatment and accessing the resources you need to begin your recovery journey. Don’t hesitate to contact us for more information.
Our admissions team is here to assist you with verifying your insurance coverage in a quick and efficient manner. To get started, we will ask for your policy number and provider details, which we will use to contact your insurance provider and learn about your coverage options for our treatment services.
Through our insurance verification process, we will confirm the specifics of your plan, the types of care covered by your insurance, and any out-of-pocket costs or deductibles you may be responsible for. Our process is entirely confidential and will not have any impact on your insurance, employment, or personal situation.
Navigating the insurance process can be challenging, but we are committed to making it as simple and stress-free as possible. Our team is here to help you better understand your coverage and make informed decisions about your treatment options. Contact us today to learn more about our insurance verification process and how we can assist you in your journey toward recovery.
At The Recovery Team, we accept a wide variety of health insurance plans, including individual policies purchased under the Affordable Care Act (ACA), as well as employer-sponsored policies. Additionally, we also accept some state-funded insurance policies, based on their coverage.
Our experienced team of insurance experts is available to answer all your questions and verify your insurance coverage. If you would like to learn more about the types of insurance we accept, you can visit our website’s insurance section located in the menu.
We believe that access to addiction treatment should be available to everyone, regardless of their financial situation. Our commitment to working with different types of insurance plans is part of our mission to provide high-quality care and support to those struggling with addiction. Contact us today to learn more about our services and how we can help you on your path to recovery.
In the event that you do not have health insurance, The Recovery Team provides competitive self-pay and scholarship options. Our team is available to provide you with all the necessary information about our services to help you make an informed decision.
We understand that seeking addiction treatment can be daunting, especially when considering the costs associated with it. That is why we offer self-pay and scholarship options that are designed to be both affordable and accessible.
If you would like to learn more about these options, please don’t hesitate to contact our center. Our staff is available to answer any questions you may have and provide you with the support you need to make the best decision for yourself or your loved one. Let us help you take the first step toward a healthier and happier life.
It’s important to note that while most insurance plans cover the cost of addiction and mental health treatment, the extent of coverage can vary depending on the specific plan. That said, there are certain types of services that are commonly covered, such as outpatient care, inpatient care, and therapy sessions.
At The Recovery Team, our team of insurance experts can help you navigate the specifics of your plan and determine the types of services covered, so you can make informed decisions about your care.
Insurance coverage is typically available for addiction and mental health-related assessments, which may include visiting our facility, meeting our staff, and undergoing a full psychological or physical evaluation.
These assessments are crucial in determining the best course of treatment for each individual’s unique needs, and at The Recovery Team, we are committed to working with a range of insurance providers to make these assessments accessible to everyone seeking help.
Most insurance plans cover the cost of working with a licensed psychiatrist to address substance use disorder and addiction. At The Recovery Team, we are proud to have a team of professional medical experts who are licensed and certified to provide top-quality care and support to our clients.
We understand the importance of mental health and substance abuse services, and we are committed to working with insurance providers to ensure that our services are recognized and accessible to those in need.
Individuals who require detoxification from drugs or alcohol typically have coverage for this service. In many cases, insurance will cover the cost of care at a detox facility, where patients receive 24/7 medical supervision as they break their chemical dependence. Detox services are essential for both emergency cases and those who are taking their first step toward recovery.
Inpatient and residential care are popular forms of treatment that require patients to live at the treatment center while receiving therapy and learning new skills from trained professionals. During their stay, patients receive comprehensive care tailored to their specific needs.
The length of time spent in residential care is determined by the severity of the individual’s condition and can vary from person to person. Our team of insurance experts is available to verify your plan and determine the potential length of your stay.
At The Recovery Team, we are committed to providing the highest quality care and support to all our clients, regardless of their insurance coverage.
Outpatient treatment differs from inpatient care in that it involves visiting our facility for therapy sessions and then returning home. Our team of insurance experts can verify your outpatient benefits, which are typically covered by most insurance plans. Unlike inpatient care, outpatient treatment allows you to continue with your daily activities while receiving treatment for addiction or mental health issues.
At The Recovery Team, we are committed to finding the best treatment options that suit your specific needs. Our dedicated and confidential team will provide you with answers to all of your questions.
In the event that we cannot assist you, we will gladly offer you a referral to another rehab facility that accepts your coverage. Contact us today at (800) 817-1247 to learn more about our services and verify your insurance.

Discover expert tips for repairing family relationships and fostering healthy connections with The Recovery Team.

Discover practical tips on how to set boundaries with people in this expert guide from The Recovery Team.
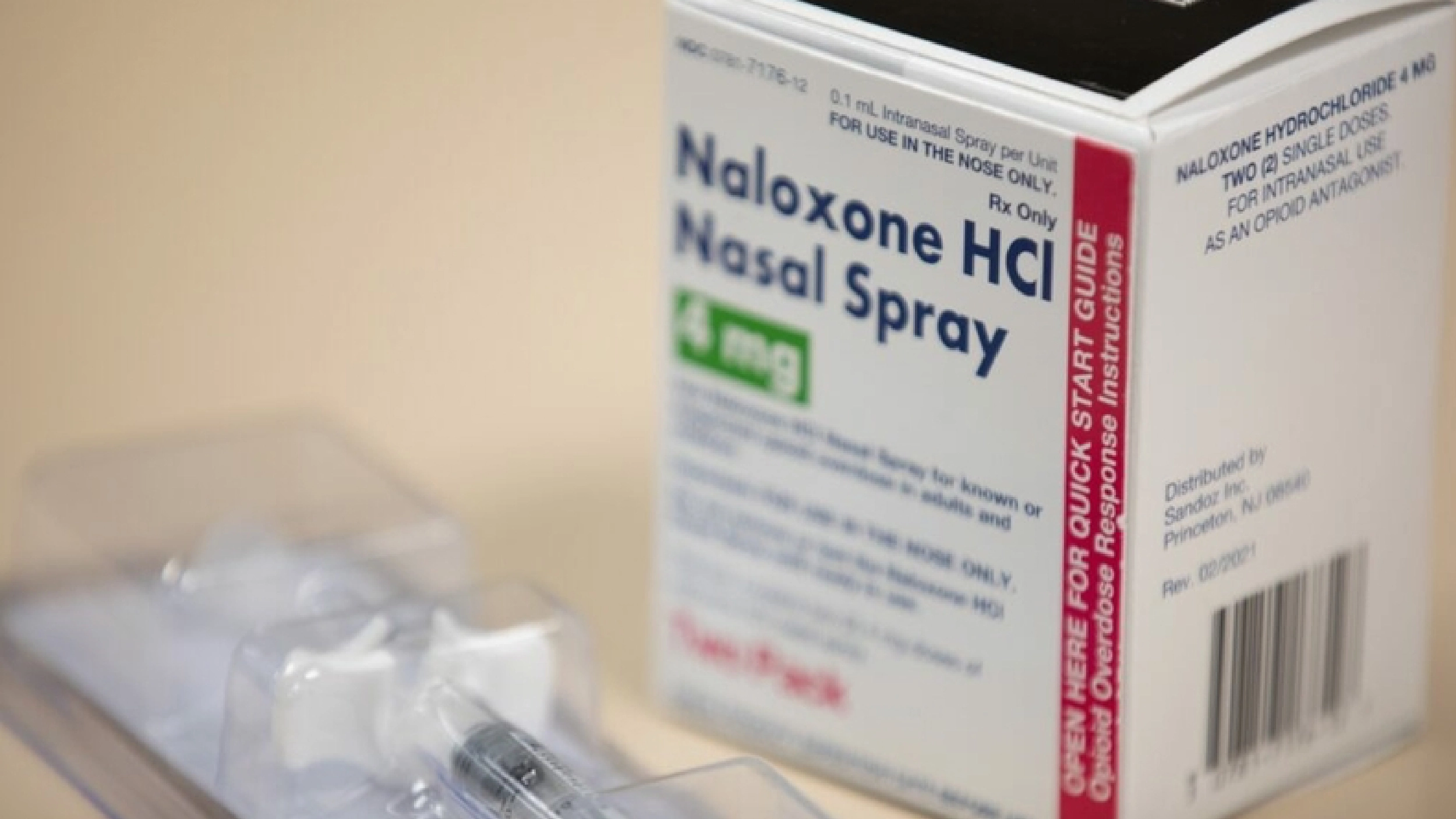
Naloxone saves lives. The Recovery Team shares how to reverse an opioid overdose with this drug.